Recent Posts
What’s the difference between inflammatory bowel disease and irritable bowel syndrome?

Receiving a diagnosis from your health care team can be difficult. You may only hear parts of the conversation as your mind starts to think about what treatment will be necessary or how this will affect your daily life.
When receiving a diagnosis related to gastroenterological conditions, misinterpreting the diagnosis can have a radically different meaning between similar-sounding conditions. This is true for inflammatory bowel disease, or IBD, and irritable bowel syndrome, or IBS.
What is inflammatory bowel disease?
Inflammatory bowel disease is a group of autoimmune diseases that run the spectrum from ulcerative colitis to Crohn's disease. Inflammatory bowel disease is a dysregulation in the body where the immune system attacks the bowel and causes inflammation.
The onset of inflammatory bowel disease may be triggered by a combination of a genetic predisposition and an illness or exposure to something in your environment that causes the immune system to attack the bowel and create inflammation.
Inflammatory bowel disease has two peak times for diagnosis in adults: people in their early 20s to 30s and people in their 50s and 60s.
Common symptoms you may experience with inflammatory bowel disease are:
- Diarrhea
- Rectal bleeding
- Bloating
- Occasional constipation
- Gas
- Urgent bowel movements
- Cramping abdominal pain
Symptoms of inflammatory bowel disease may be experienced regularly and can significantly affect your quality of life. The treatment for inflammatory bowel disease is multifactorial. Treatment typically involves using immunosuppressive drugs to help the immune system avoid attacking the bowel. Dietary modifications can decrease inflammation.
It's OK to talk about irritable bowel syndrome
You should not feel embarrassed discussing the symptoms of irritable bowel syndrome with your health care team. As many as 1 in 5 adults in the U.S. have signs and symptoms of irritable bowel syndrome; yet, fewer than 1 in 5 who have these symptoms seeks medical help.
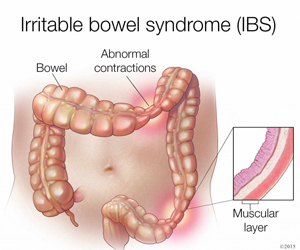
Irritable bowel syndrome is a functional bowel disorder that causes your digestive organs to look normal but not function normally. For most people, irritable bowel syndrome is a chronic condition that can fluctuate from producing mild to severe symptoms. Sometimes symptoms disappear entirely.
While irritable bowel syndrome can affect almost anyone, certain risk factors exist, including people who are:
- Young
- Female
- Have a family history of irritable bowel syndrome
- Have a history of anxiety or depression
Living with irritable bowel syndrome
While irritable bowel syndrome cannot be cured, it doesn't permanently harm the intestines and doesn't cause cancer. Irritable bowel syndrome may affect your quality of life, so it's important to learn about your symptoms and what you can do to control them.
The current understanding of irritable bowel syndrome indicates hypersensitivity in the gut causes the symptoms. This affects how your body perceives stimuli related to bowel function. Treatment focuses on relieving symptoms so you can live as normally as possible.
In most cases, you can successfully control mild symptoms of irritable bowel syndrome by learning to manage stress and making healthy changes to your diet and lifestyle. This includes exercising regularly, drinking plenty of fluids and getting enough sleep. Your health care team may prescribe other specific dietary changes, medications and supplementary treatments.
While living with irritable bowel syndrome can present daily challenges, your health care team is available to help. They can guide you through an appropriate evaluation of your symptoms and provide treatments to help you optimize your quality of life.
Daisy Batista, M.D., is a gastroenterologist in La Crosse, Wisconsin.