Recent Posts
COVID-19 care generates gratitude, new career

It was Thanksgiving week in 2021 when April Alden-O'Connor's life took an unimaginable turn. She'd spent a crisp November day deer hunting with her brother. While she was away, her boyfriend, Joe Houske, told her he'd tested positive for COVID-19.
Joe and April isolated at their home in Hastings, Minnesota. But by Friday, Nov. 26, April, who was 30 at the time, developed symptoms. On Sunday, she tested positive for COVID-19.
Unlike Joe, April's symptoms were worse — way worse. "I felt like death warmed over and was having trouble breathing," April says.
As her symptoms worsened, including her blood oxygen dropping to 70%, April sought care in the Emergency Department at Mayo Clinic Health System in Cannon Falls, followed by being admitted to the hospital on Dec. 2 at Mayo Clinic Health System in Red Wing.
From ICU to ECMO
April's condition continued to deteriorate. On Dec. 8, she was transferred to the ICU at Mayo Clinic Hospital — Rochester, Methodist Campus, where she was told she needed to be intubated.
"I texted my mom that there must be a misunderstanding. Then I asked to call my family so I could say goodbye, knowing that I might not wake up on this side of the living," she says.
By Dec. 15, April had developed severe COVID-19 pneumonia. To accelerate her care and take the pressure off her heart and lungs, April's care team approved her for extracorporeal membrane oxygenation, or ECMO, the highest form of life support, which required another transfer, this time to Mayo Clinic Hospital — Rochester, Saint Marys Campus.
"The next thing I remember was slowly waking up around Christmas," she says. "I was heavily medicated and experiencing weird hallucinations, like thinking I had six babies. When I asked for them, my care team thought I meant our dogs."
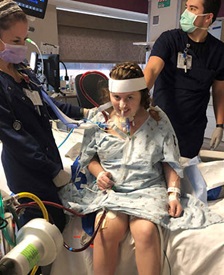
The coming weeks were rough. April was treated for COVID-19 pneumonia and bacterial pneumonia, a staph infection and sepsis. But then her condition began improving and the infections were brought under control. On Jan. 21, 2022, April was taken off ECMO. However, she first had to prove she could walk around the unit with assistance.
"My favorite physical therapist cheered me on, but it still took about eight people to help me walk," April says.
On Jan. 24, she'd passed the next test: the ability to swallow.
"I'm a big water drinker, and I drank nine glasses of water. It felt wonderful," she says. That same day, she was moved from the ICU to the respiratory unit, then to the general floor.
Deep gratitude for care
On Feb. 3, April was discharged home on oxygen. By the end of June, her lungs were recovered enough to stop the supplemental oxygen.
April's COVID-19, 63-day journey by the numbers was: 48 days in the ICU, 38 days on ECMO and 50 days being unable to speak.
Looking back, she feels deep, lasting gratitude for the care she received, including the:
- Nurse who braided her hair across the top of her head so it was out of the way.
- Therapists and nurses who helped her cope with the hallucinations, anxiety and post-ICU post-traumatic stress disorder.
- Nurses who sat with her and held her hand so she knew she wasn't alone.
- Physical therapists who helped her rebuild strength.
- Respiratory therapists who monitored and coached her while her lungs healed.
- Scores of health care professionals and aides who oversaw her care and made her as comfortable as possible.
Finding a new path
April still doesn't feel completely recovered. She continues to experience hair loss and undergo pulmonary rehabilitation. The smell of hand sanitizer and beeping machines trigger memories of her hospital stay. But she knows she's made gigantic strides, including returning to the dance studio where she studied tap and jazz for nearly 15 years.
Before COVID-19, April was a personal care assistant, but dreamed of becoming a nurse like her mom, who retired in December 2022 after 40 years at Mayo Clinic. But April suffered from such severe migraines that college seemed impossible.
"Maybe God thought I'd been through enough, but for the past seven or eight months, the severity and frequency of my migraines has decreased significantly," she says.
In November 2022, she took a first step toward a new career. She applied and was hired for a scheduling desk position at Mayo Clinic Health System in Cannon Falls.
"It's a big job, but I love interacting with people, especially the elderly," April says. "Nursing may still be in my future, but I want to regulate my life a bit first. But becoming a nurse seems more possible now than ever."
Moving forward
From her COVID-19 experience, April admits it may be a cliché, but she now realizes life is precious and no one is promised unlimited time.
"I learned not to suffer in silence, but to seek help when I need it. I strive to breathe deeply, practice mindfulness and, most importantly, reach out to others. Tell people you love them, spend time with them doing things you love and spend less time on what doesn't serve you."
And one more insight she offers: If someone you know is in a similar life-threatening situation, keep a journal for them detailing their care.
"It's helpful to know the details and clarify what happened. It's part of the healing," April says.





