When you need it most.
Expert surgical care
Need to make an appointment?
Recent Posts
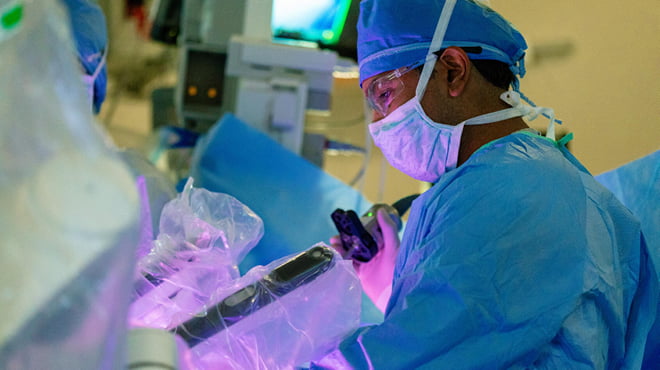
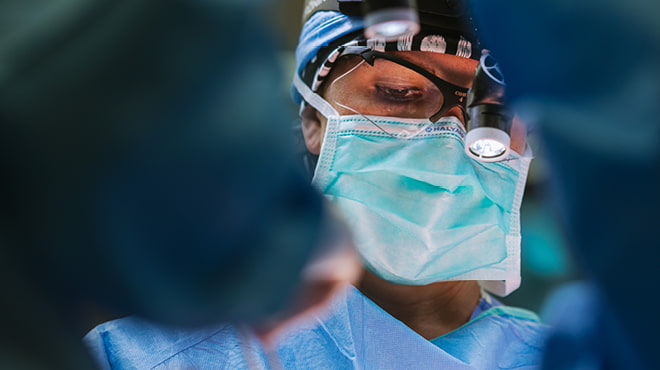
Surgery in La Crosse
Having surgery is a major event in your life. We know this and make every effort to keep you as comfortable as possible, focusing on you as an individual.
Our surgeons and staff in La Crosse, Wisconsin, work as a coordinated team treating a wide variety of illnesses ranging from simple to complex. We offer comprehensive, advanced care and service to every patient, including children. A certified child life specialist from Pediatrics in Onalaska typically is available to help children and their family members cope with the stress and uncertainty of having surgery.
Surgical conditions and treatments
We offer a wide range of surgical treatments for a multitude of conditions to help improve your daily life, including:
- Breast
- Colon and large/small intestine
- Endocrine
- Gallbladder
- Hernia
- Pancreas
- Skin
- Stomach
- Ulcers
- Vascular system
Breast
- Cysts, lumps, cancer, nipple discharge
- Stereotactic breast biopsy
- Sentinel lymph node biopsy and axillary dissection
- Lumpectomy
- Mastectomy
- Skin and nipple sparing breast removal
- Prophylactic mastectomy
Colon and large/small intestine
- Appendicitis
- Colorectal polyps and cancer
- Diverticulitis
- Endoscopy
- Intestinal obstruction
- Small bowel cancer
Endocrine
- Adrenal nodules
- Parathyroid removal
- Thyroid cancers
- Thyroid nodules and cysts
Gallbladder
- Gallbladder dysfunction
- Gallstones
Hernia
Pancreas
Skin
Stomach
Vascular system
- Carotid artery disease
- Peripheral vascular disease (PAD)
- Vascular bypass (surgery to legs)
- Abdominal aortic aneurysm
- Endovascular aortic repair (EVAR)
- Venous Insufficiency
- Varicose veins
Additional surgical services available in La Crosse:
Locations in La Crosse
Not all treatments, tests and services are available at all Mayo Clinic Health System locations. Check with your preferred location in advance.

Clinic
- Surgery Hours:
- Mon-Fri:8:00 AM - 5:00 PM
Directions
800 West Ave. S., La Crosse, WI 54601
- Appointments:
- 608-392-9883
Providers View More
Not all treatments, tests and services are available at all Mayo Clinic Health System locations. Check with your preferred location in advance.