made personal
Recent Blogs
Breast Cancer Care Services & Treatments
Changes to your breast or a breast cancer diagnosis can cause a lot of worry. You need fast, accurate answers only expert medicine can provide. Our breast cancer experts provide comprehensive care — from diagnosis through treatment and survivorship — tailored to your needs. Innovative technology and coordinated care help speed up evaluation, reduce uncertainty and simplify each step of your breast cancer journey.
Are you a new patient with concerns about your breast health?
We make it easy for you to request an appointment.
Existing patients should schedule through the patient portal.
If you're feeling unsure about your breast cancer diagnosis, a second opinion from an expert can be important for your peace of mind. We can provide answers to the questions you may have about your medical diagnosis or treatment plan. No referral is required.
Find out more about our breast cancer care services:
- Conditions and consultations
- Diagnosis and treatments
- Breast cancer care specialists
- Referrals
- FAQ
- Breast cancer care locations near you
- Breast cancer care specialists near you
Conditions and consultations
Any breast symptoms — such as a breast lump, nipple discharge or breast pain — should be evaluated, even if a recent mammogram was normal. Not all breast changes are caused by cancer, but prompt evaluation helps guide next steps.
Conditions we treat include:
- Breast cancer
Cancer that forms in breast tissue and can affect people of all genders. Breast cancer varies in type, stage and treatment approach. Breast cancer is the most common cancer diagnosed in women in the U.S. Care is tailored based on factors such as tumor type, stage, genetic risk and overall health. - Breast cysts
Fluid‑filled sacs in the breast that may cause tenderness or feel like a lump. Most breast cysts are benign. Breast cysts can change with hormonal cycles and may vary in size. Evaluation helps determine whether follow‑up or additional imaging is needed. - Fibroadenoma
A firm, smooth, rubbery breast lump that is usually noncancerous and more common in younger people. Fibroadenomas are often discovered during imaging or physical exams and are monitored or treated based on size, symptoms and patient preference. - Mastitis
Breast inflammation that can cause pain, swelling, warmth and redness, often related to blocked milk ducts or infection. Mastitis commonly occurs during breastfeeding but can affect others. Early treatment helps relieve symptoms and prevent complications. - Papilloma
A growth within a milk duct that may cause nipple discharge or a small lump behind or near the nipple. Papillomas are typically benign but often require imaging or biopsy to confirm diagnosis. - Atypical hyperplasia
An accumulation of abnormal cells within breast tissue identified through biopsy after abnormal imaging or exam findings. Atypical hyperplasia is not cancer but may increase future breast cancer risk, prompting closer monitoring or preventive strategies.
Diagnosis and treatments
Your care begins with a thorough evaluation to understand your symptoms and diagnosis. Based on findings, your care team develops a personalized plan using advanced diagnostic tools and treatment options.
Diagnostic and evaluation
- Breast cancer screening and evaluation
Breast cancer diagnosis may begin with imaging, physical exams or additional testing based on symptoms and risk factors. Evaluation is tailored to you and may include screening or diagnostic imaging, biopsy or referral to a breast specialist. - Advanced breast imaging technology
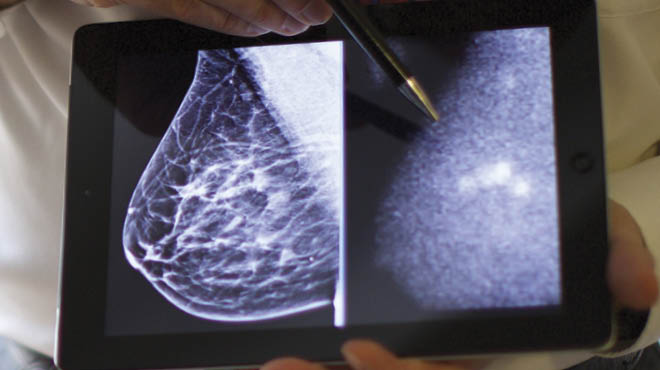
Imaging helps detect and evaluate breast changes with accuracy and clarity. Options may include 3D mammography (tomosynthesis), breast MRI, contrast‑enhanced digital mammography and molecular breast imaging (MBI). Computer‑aided detection (CAD) technology may be used during mammography to assist radiologists by analyzing images for areas that may need closer review. - Image-guided breast biopsy
Biopsies help determine whether breast changes are benign or cancerous and may be guided by ultrasound, stereotactic imaging or MRI, depending on findings.
Treatments we provide
- Surgical care
Surgery may be used to remove cancer or evaluate breast changes. Options may include lumpectomy, mastectomy or breast reconstruction surgery. - Bioimpedance screening and lymphedema management
- Radiation therapy
Radiation therapy uses targeted treatment to destroy cancer cells and reduce recurrence risk. Radiation plans are individualized based on cancer type, stage and surgical outcomes. - Medical therapies
Medications may be used alone or in combination to treat breast cancer. Treatment options may include chemotherapy, hormone therapy and infusion‑based therapies. - Genetic counseling and testing
Genetic counseling helps assess inherited cancer risk and guide personalized care. Counseling may be recommended for people with a strong family history or certain cancer characteristics. - Supportive and integrative care
Supportive services help manage symptoms and improve quality of life during treatment. Services may include bioimpedance screening and lymphedema management, scalp cooling caps, and integrative approaches for symptom support. - Clinical trials and cancer research
Clinical trials may offer access to emerging treatments. Participation is based on eligibility and availability and is always voluntary. - Mobile Mammography
Mobile mammography may be available in select communities to improve access to breast cancer screening. - Pharmacogenomics and medication management
- Scalp cooling cap to prevent hair loss
As part of our comprehensive cancer approach, additional diagnostic tools and treatment plans may include options available at Mayo Clinic.
Breast cancer care specialists
You’ll receive care from a coordinated, multidisciplinary team that may include specialists in breast imaging, surgery, oncology, radiation oncology, genetics and supportive care — all working together to support you through every step of care.
Our specialists include:
- General surgeons
- Infusion therapists
- Nurse navigators
- Oncologists
- Plastic and reconstructive surgeons
- Primary care providers
- Radiology breast technicians
Additional care and therapies may be provided by:
- Medication therapy management
- Nutrition counseling
- Pathology
- Physical therapy and occupational therapy
- Radiation oncology
- Research
- Social services
- Surgery
Referrals
You can make an appointment without a referral from your provider — simply call the appointment number of your preferred breast cancer care location.
FAQ
Should breast symptoms be evaluated even if my mammogram was normal?
Yes. Any breast symptoms — such as a new lump, nipple discharge or breast pain — should be evaluated, even if a recent mammogram was normal. Further evaluation helps determine whether symptoms are caused by a benign condition or require additional testing.
What imaging tests may be used to evaluate breast cancer?
Breast cancer evaluation may include imaging such as mammography, breast ultrasound, breast MRI or molecular breast imaging (MBI), depending on your symptoms, risk factors and prior imaging results. Your care team will determine which imaging is appropriate for you.
What is dense breast tissue?
Dense breast tissue refers to the amount of fibrous and glandular tissue compared to fatty tissue in the breast, which is visible on a mammogram. Breast density is common and not abnormal. Your healthcare team can explain what breast density means for you and whether additional imaging or follow‑up is recommended based on your individual situation.
What is a breast MRI?
A breast MRI is a type of imaging that uses magnets and radio waves to create detailed images of breast tissue. It may be used in certain situations to provide additional information beyond mammography or other imaging, based on individual risk factors or findings.
What is molecular breast imaging (MBI)?
Molecular breast imaging (MBI) is a type of breast imaging that may be used in certain situations to help evaluate breast changes. It involves using specialized technology to detect areas of increased activity within breast tissue and is sometimes used in addition to mammography or other imaging based on individual needs.
What is lymphedema and how is it related to breast cancer care?
Lymphedema is swelling that can occur when lymph fluid does not drain properly, sometimes as a result of breast cancer surgery or radiation therapy. Evaluation and management of lymphedema may be part of supportive breast cancer care, based on individual needs.
What does a multidisciplinary breast cancer care team mean?
A multidisciplinary breast cancer care team brings together specialists from areas such as breast imaging, surgery, oncology, radiation oncology and genetics to evaluate your care together and develop a coordinated treatment plan tailored to your needs.
How does Mayo Clinic Health System ensure quality breast cancer care?
Breast cancer care at Mayo Clinic Health System is guided by nationally recognized standards and a coordinated, team‑based approach to diagnosis and treatment. Care is tailored to each person’s needs and may include access to advanced imaging, specialty care and supportive services.
What should I expect during breast imaging or diagnostic tests?
Imaging exams are performed by trained technologists in private clinical settings. Your care team will explain each step of the exam, answer questions and guide next steps based on results. The type of imaging you receive depends on your individual situation.
What should I expect during my first appointment, and what should I bring?
For your first appointment, bring any imaging or medical records from non-Mayo Clinic Health System facilities. Complete a medical records release form to authorize the transfer of health records from another health care facility to us. Visit our Medical Record Forms page for this form and other forms in multiple languages.
What are my payment options, and do you offer financial assistance?
Visit the billing page of your preferred location for information on insurance, billing and payments.
We serve patients in difficult financial circumstances and offer financial assistance to those who have an established need to receive medically necessary services. Learn more about financial assistance options.
Can you provide a second opinion?
Yes — simply call the appointment number at your preferred breast cancer care location. See What should I expect during my first appointment? for tips on how to prepare.
Do you have an after-hours number in case of emergency?
Always call 911 in case of an emergency. For after-hours help with other issues, get virtual care 24/7 through the Primary Care On Demand app or review our convenient care options.
Explore our locations or providers near you for details on expert breast cancer care:
Locations View all breast cancer care locations

Austin, MN
Hospital and Clinic- Building hours:
- Mon-Fri:5:30 AM - 8:00 PM
- Emergency Department Hours:
Open 24 hours
- Appointments:
- 507-433-8758
- General:
- 507-433-7351

Menomonie, WI
Hospital and Clinic- Hours:
- Mon-Fri:8:00 AM - 5:00 PM
- Appointments:
- 715-838-6072

Eau Claire, WI
Luther Campus Clinic- Hours:
- Mon-Fri:8:00 AM - 5:00 PM
- Appointments:
- 715-838-6072

Albert Lea, MN
Hospital and Clinic- Building hours:
- Mon-Fri:6:00 AM - 7:30 PM
- Emergency Department Hours:
Open 24 hours
- General:
- 507-373-2384
Providers View More





Related Upcoming Classes & Events View More
Look Good Feel Better – Helping Women with Cancer
The workshops offer tips and tools for helping women with cancer look good and feel better.